What's the Difference Between a D.O. and an M.D.?
February 8th, 2023 | 3 min. read
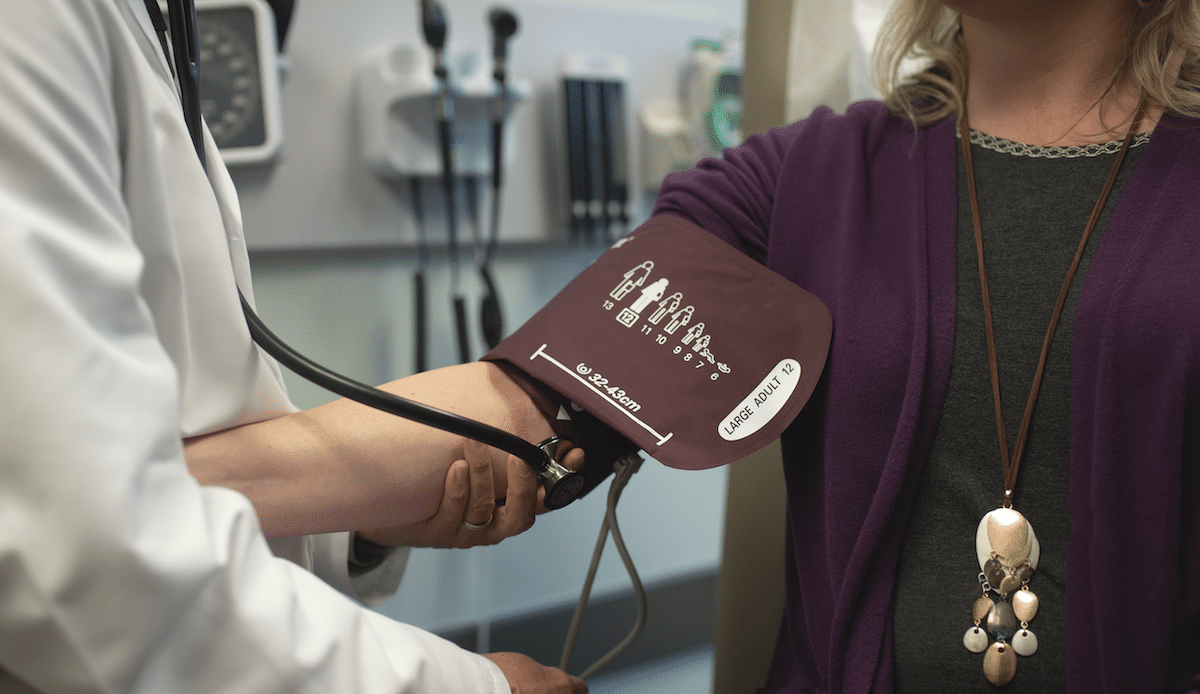
Typically, when doctors are referenced, you’re likely to hear “M.D.” associated with the doctor’s name. And this makes sense because roughly 89% of physicians in the U.S. are medical doctors (M.D.).
But wait … what about that other doctor?
About 11% of physicians in the U.S. are what’s known as a D.O. or doctor of osteopathy. While still limited, the number of doctors of osteopathy has increased by 81% in the last decade.
If you're looking for a new primary care physician, you may run into both. Both degrees mean that the doctor is a licensed physician. There are a few differences in training and philosophy but for patients, there’s virtually no difference between treatment by a D.O. vs M.D.
Just like with the gender of your physician or internal medicine vs. family medicine, you can be confident in the care you get from just about any doctor, whether they are a D.O. or an M.D. Let us explain why.
What is a Doctor of Osteopathy (D.O.)?
If the term isn’t familiar to you, you’re not alone. In fact, I was a pre-med student researching medical schools when I first remember hearing about this way of practicing medicine. After I learned more, I applied only to schools offering osteopathic degrees.
After medical school, both M.D.s and D.O.s must complete residency training in their chosen specialties. They must also pass a licensing examination before they can treat people and prescribe medications.
The main difference is that osteopathic medical schools also require additional classes, typically about 200 hours more, on the skeletal system (osteo comes from the word meaning “bone”) and the interactions of the body with diseases.
Because of this training, a D.O. tends to address medical conditions from both a medical and lifestyle perspective. Doctors of Osteopathy are known for placing an emphasis on getting to know a patient’s lifestyle, family, and unique concerns, which informs medical treatment.
Whether it’s a chronic disease or an everyday cough, D.O.s are likely to ask about the medication you’re taking, and also what you are eating, how much stress you’re feeling at work, and how you are sleeping. D.O.s are trained to ask questions like these to gain a full understanding of a patient’s lifestyle, which can ultimately impact their health.
D.O. vs M.D: The Similarities
Let's start with the similarities between a doctor of osteopathy and a medical doctor.
- Both M.D. and D.O. physicians base diagnosis and treatment recommendations on scientifically-proven conclusions.
- Both attend four years of medical school, plus a residency program ranging from three to seven years.
- Both are licensed by the same state licensing boards. In other words, both M.D.s and D.O.s must meet the same requirements to practice medicine.
- Both can practice medicine in all 50 states.
- Both are found in every type of specialty medicine.
- Both follow the same undergraduate academic path – a bachelor’s degree, pre-med coursework, and taking the MCAT.
Difference Between D.O. and M.D.: Allopathic vs. Osteopathic
A medical doctor, or M.D., is a doctor of allopathic medicine. Though we rarely use the term allopathic in daily conversation, it refers to the “classical” form of medicine that focuses on the diagnosis and treatment of human diseases, typically by observing the symptoms presented by the patient.
A D.O. practices osteopathic medicine. In this style of practice, doctors are trained to take a more holistic view of medicine in which the focus is on seeing the patient as a whole person to reach a diagnosis, rather than observing the symptoms alone.
Keep in mind that we are talking only about how these two types of physicians are trained. Many M.D.s also approach patient care from this “whole person” perspective.
Why I Chose Osteopathic Medicine
As a pre-med student, I was drawn to the philosophy of osteopathic medicine. I believed then, and still do, that this more holistic approach to care was more open-minded and could provide a more nuanced understanding by considering the patient’s full life.
The programs were virtually the same in terms of training and requirements, so why not take advantage of the additional classwork? The additional knowledge could only benefit me as a physician and by extension, my patients.
Being a part of PartnerMD allows me to bring this style of practice to my patients in a more hands-on and meaningful way. I have more time with patients to get to know them and their lifestyles.
As a result, the recommendations I am able to make are much more personal to each individual that I treat.
I have time to explain why I making a specific recommendation and how to implement it. We have the time to talk about eating clean, avoiding environmental toxins, and how to keep yourself healthy in an unhealthy world.
Find the right concierge doctor for you at PartnerMD.
If you are frustrated by today’s typical healthcare experience, come meet with a PartnerMD physician. You can check out all of our physicians here.
At PartnerMD, we believe hassle-free primary care is only the foundation of a better healthcare experience.
When you join PartnerMD you get greater access to a great doctor, but that's just the beginning. You get access to the most customizable advanced physicals to help identify hidden vulnerabilities to your health. And you get access to certified health coaches who provide expertise and accountability to support a healthy lifestyle.
All that is wrapped up in one concierge medicine membership designed to provide better healthcare for an even better you.
Topics:

